Minimally invasive surgery – otherwise known as laparoscopy – has become incredibly common in recent years for a variety of medical procedures. The surgical method consists of making a small incision across the stomach and inserting a lighted tube or scope, along with other needed tools, to access whatever organs are the focus of a procedure.
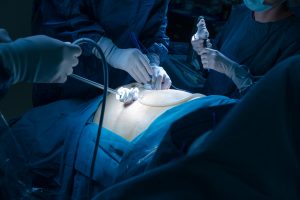
The benefits of laparoscopy often result in an easier recovery for patients, leaving them with smaller surgical scars, less painful healing and shorter hospital stays. The minimally invasive method of surgery can be used on a wide array of surgeries, including those involving the appendix, spleen, colon, gallbladder, liver, pancreas, esophagus, small intestine and stomach. It’s also used to repair hernias, remove smaller tumors or cysts and close a woman’s fallopian tubes.
Outside of smaller, rural hospitals, most medical centers today have both the technology and surgical expertise to conduct the majority of these minimally invasive procedures. Sedro-Woolley’s PeaceHealth United General Medical Center is no exception.
Doctor Farabi Hussain, a surgical oncologist who recently joined the PeaceHealth United General team after 20 years of practicing medicine in California, is an expert in minimally invasive spleen, colon, pancreas and liver surgeries. Hussain says minimally invasive surgery has improved significantly in both scope and quality in the time he’s been a doctor. “There are now liver surgeries that are being done completely laparoscopically,” he says. “Things have advanced very quickly and people have accepted the technology and the methodology of doing laparoscopic surgery. It’s really blossomed in the last 20 years.”
So who’s a good candidate for this kind of surgery? Hussain says that depends on the patient. If someone has already had multiple open abdominal surgeries, or is otherwise more easily prone to injury, they might want to consider more traditional surgical methods. The same goes for those with larger hernias, cysts or tumors. In any case, Hussain says proper discussion must be had between a patient and their providers. “It really has to be well thought-out between the surgeon and the patient,” he says. “We have to look at and decide whether it’s a safe operation for them or not.”
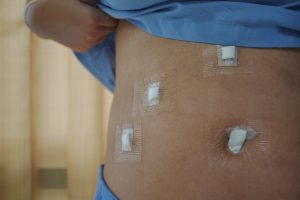
For those who are good candidates, in-hospital recovery time is generally shorted by about 24 hours, saving them money on medical costs and getting them back to the comforts of home recovery quicker. Typical scars from minimally invasive surgery are also small, generally no bigger than half an inch long. Again, though, this all depends on the type of procedure and the individual patient. “Gallbladder patients, you send them home the same day you operate,” Hussain says. “Appendix patients usually go home the same day. A colon patient may go home in three days with laparoscopic surgery, and with an open procedure they might go home in four or five.”
Hussain says gallbladder, appendix and some colon-based laparoscopic surgeries can be done at PeaceHealth United General, while more complex procedures are better conducted at Bellingham’s PeaceHealth St. Joseph Medical Center.
In addition to conducting minimally invasive and other general surgeries, Hussain is putting his extensive skill as a surgical oncologist to work in Skagit County. After conducting his clinical fellowship for surgical oncology at Harbor-UCLA Medical Center, Hussain spent two decades at San Bernardino County Medical Center. There, he was responsible for complex gastrointestinal, lung and rectal surgeries, and served as a supervising physician for residents. He also provided clinical training to medical students in general surgical residency programs.
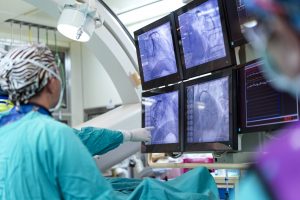
Hussain’s practice has paid special attention to breast, pancreatic and liver cancers, and he’s already conducted several breast and melanoma surgeries since starting at PeaceHealth United General in January. Being a doctor on the frontlines of the battle against cancer, he says, is something he relishes. “I really enjoy working with cancer patients,” he says. “Sometimes it’s good, sometimes it’s not. It gives me a lot of satisfaction to see them often times get better. Being there for the patients is very fulfilling.”
For more on the array of surgical care available at PeaceHealth United General Medical Center, visit the PeaceHealth website.
Care in a time of COVID-19
Staying home during the COVID-19 pandemic has helped flatten the curve of this health care crisis. But it has also meant delaying care for many people. We continue to follow guidelines established by the Centers for Disease Control and Prevention and the Washington state Department of Health while we work to minimize delays in care brought on by the pandemic. PeaceHealth remains committed to providing the care our patients depend upon and we continue to take steps to keep you safe when you visit. For more information about what we’re doing to protect our patients, please visit the PeaceHealth website.
Sponsored



































